2015-12-27
Equine Sarcoids
Equine sarcoids are a very common locally invasive fibroblastic skin tumor. There are six distinct sarcoids that are classified according to their appearance and clinical behavior.
- Occult – this sarcoid is flat, no hair (alopecia) and may have mild scaling.
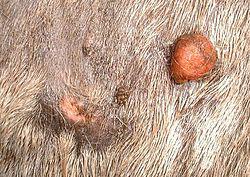
- Nodular – firm, well defined subcutaneous (under the skin) lesions.

Haired occult sarcoid on the left and nodular sarcoid on the right - Verrucous – wart like, raised, scaly, with a lichenified appearance and thickening of the skin (epidermis).

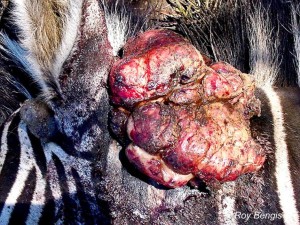
- Fibroblastic – fleshy, ulcerated with local infiltration of the surrounding skin.

- Mixed – may include any, or all, of the above mentioned forms. These sarcoids often become progressively more aggressive.

- Malevolent – this is the most infrequent form. This form proliferates rapidly and may spread along fascial planes and vessels.
The bovine papillomavirus are causally associated with the development of equine sarcoids. Although it is widely accepted that bovine papillomavirus (BPV) is necessary for sarcoid development, infection alone is not sufficient for tumor development. Many studies have suggested there is a breed predilection, with Quarter Horses, Arabians, and Appaloosas having an increased risk. Horses with certain equine leucocyte antigen (ELA) haplotypes appear to be at a higher risk for sarcoid development. Even though many horses have the ELA, they do not always develop sarcoids; therefore researchers have determined that other factors are involved. Sites of skin trauma or open wounds are more likely to develop sarcoids. Although little is known about how this disease is spread, one potential mechanism is that flies or other insects may act as vectors.
Diagnosis
A presumptive diagnosis is commonly based on the appearance of the growth. A definite diagnosis requires a biopsy or histopathology. However, biopsy induced trauma may exacerbate the sarcoid and result in the sarcoid becoming larger.
Treatment
Unfortunately, there is no one uniformly effective treatment for equine sarcoids. There are several routes of therapy. Contact Arizona Equine for more information.
- Surgical excision – this method is utilized for tumors are easily accessible and in a location allowing closure of the skin. It is critical that wide margins around the tumor be removed to decrease the incidence of reoccurrence. Reoccurrence is thought to occur due to latent BPV present in the surrounding normal skin that is disrupted and activated by surgical trauma.
- Laser removal – this is a surgical instrument that cuts and vaporizes soft tissue. The success rate of tumor removal with the laser is higher (60 -80% per some researchers). The higher success rate may be due to decreased disruption of quiescent tumor cells when compared to scalpel removal.
- Cryotherapy – this method involves the use of liquid nitrogen ( -196 degrees centigrade) which destroys tumor cells through the formation of intracellular ice and subsequent rupture of the cell when the ice crystals thaw. Often cryotherapy is combined with surgical excision.
- Hyperthermia – a radiofrequency hyperthermia device is held against the tumor and heated to 50 degrees centigrade for 30 seconds. The tumor cells are preferentially destroyed due to the fact that these cells are disorganized and often have a compact vascular pattern. With this pattern, the tumor has difficulty dissipating heat and the individual cells die. Only tumors less than 1.0 cm in diameter can be treated with this method.
- Radiotherapy – utilizes radiation to kill the tumor cells by damaging DNA and protein. There are two forms of radiotherapy, teletherapy and brachytherapy. Teletherapy is expensive and of limited availability. Brachytherapy uses small sealed radioactive sources implanted within the tumor. Many studies revealed that brachytherapy yields relatively high success rates but tumor regrowth frequently occurs.
- Chemotherapy – Injection into the tumor with Cisplatin is commonly performed. Cisplatin inhibits DNA synthesis. Cisplatin is reconstituted and mixed with sesame seed oil and then injected into the tumor.
- Immunotherapy – relies on local immune stimulation to attack and kill the sarcoid tumor cells. The most common immunomodulatory used is Bacillus Calmette and Guerin (BCG), this is an attenuated strain of Mycobacterium bovis. Other immunomodulators used to treat sarcoids are mycobacterial cell wall extracts and systemic propionibacterial cell wall extracts.
- Topical immune modulators – such as XXTERRA is a herbal compounded cream that contains bloodroot and zinc chloride. The mechanism of this cream is to activate local immune response and kill the tumor cells.
Equine sarcoids are a significant therapeutic challenge. The most important tool is client education and early recognition of potential sarcoids. Early intervention, with a small tumor is most likely to increase treatment success and decrease treatment complications.
References
1. Carr, EA. Skin Conditions Amenable to Surgery. Equine Surgery
2. Angelos J, Oppenheim Y, Rebhun W, et al: Evaluation of breed as a risk factor for sarcoid and uveitis in horses. Anim Genet 19:417, 1988.
3. Carr EA, Theon AP, Madewell BR, et al: Presence of bovine papilloma virus DNA in equine sarcoids in horses living in the Western United States. Am J Vet Res 62:742, 2001.
4. Knottenbelt DC, Kelly DF, The diagnosis and treatment of periorbital sarcoid in the horse: 445 cases from 1974-1999. Vet Ophthalmol 3:169, 2000.
5. Carstanjen B, Jordan P, Lepage OM: Carbon dioxide laser as a surgical instrument for sarcoid therapy: A retrospective study on 60 cases. Can Vet J 38:773, 1997.
6. Byam-Cook KL, Henson FM. Slater, JD: Treatment of periocular and non-ocular sarcoids in 18 horses by intersitisal brachytherapy with iridium-192. Vet Rec 159:337, 2006.



Sorry, the comment form is closed at this time.